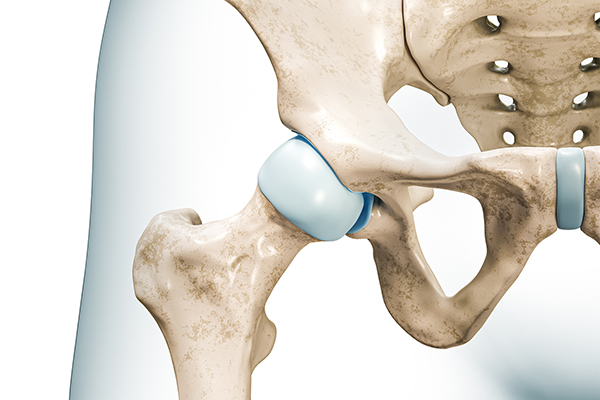
Advancements in medical technology have shifted the conversation from managing hip pain to actively restoring joint health. For young, active patients, localized cartilage damage no longer has to be the first step toward an inevitable joint replacement. Understanding the current landscape of cartilage restoration is essential for anyone looking to preserve their natural hip joint and maintain a high-level lifestyle.
From Microfracture to Advanced Scaffolding
For years, the foundational approach to cartilage restoration has been microfracture. While this remains a common first-line treatment for small defects, the science has evolved toward more durable solutions. Surgeons are increasingly using "microfracture plus" techniques, which involve placing a biological scaffold or membrane over the repair site. This helps stabilize the blood clot and encourages the body to produce a more resilient tissue that better mimics the original articular cartilage compared to traditional scar tissue.
Autologous Chondrocyte Implantation (ACI) in the Hip
One of the most significant leaps in hip preservation is the refinement of Autologous Chondrocyte Implantation (ACI). This process involves harvesting a small sample of a patient's own healthy cartilage cells, growing them in a laboratory, and re-implanting them into the damaged area. This "biologic resurfacing" aims to create hyaline-like cartilage, the specific, high-durability tissue required to withstand the immense pressures of the hip joint, offering a long-term solution that traditional methods may lack.
The Rise of "Off-the-Shelf" Cartilage Restoration
Another frontier in orthopedic science is the development of "off-the-shelf" products that can be used in a single procedure. This includes juvenile allograft cartilage fragments or dehydrated cartilage matrices that act as a "plug-and-play" filler for damaged areas. These options aim to provide the regenerative benefits of cell-based therapy without the need for a secondary surgery or a laboratory waiting period, making restorative care more accessible and efficient for the patient.
Orthobiologics as a Healing Catalyst
The science is increasingly pointing toward a "hybrid" approach, where surgical restoration is paired with orthobiologics. Integrating Platelet-Rich Plasma (PRP) or autologous cell therapy during the healing phase can act as a catalyst, providing the growth factors necessary to ensure the new tissue integrates successfully. This synergy between mechanical repair and biological support is the cornerstone of modern sports medicine.
Precision Imaging and the "Bio-Joint" Future
Looking ahead, the use of 3D printing and customized biological scaffolds is on the horizon. Surgeons are moving toward an era where we can print a biological "plug" that perfectly matches the topography of a patient’s specific cartilage defect. This level of precision, combined with our growing understanding of both joint biomechanics and biology, is leading us toward a "bio-joint" future where the need for artificial replacements may be pushed further into the future or avoided entirely.
By focusing on biological restoration today, you can maintain an active lifestyle and protect your joint's health for the years to come. Book an appointment for a clinical consultation, to explore these restorative options.